Introduction
In an age where patients have grown to the point of demanding hyper-personalized experiences on every digital channel, healthcare organizations are ramping up, but personalization in healthcare comes with a critical catch: compliance. Unlike the traditional industries in which customer data can be freely segmented and optimized, healthcare falls under the most stringent regulation, namely HIPAA (Health Insurance Portability and Accountability Act), which directs the collection, use, and sharing of patient data. This means that any HIPAA-compliant personalization must strike a fine balance between innovation and watertight safeguards around PHI (Protected Health Information).
But here is the real challenge: how do you find an easy way to personalize email marketing, how do you customize patient portals and digital care journeys without risking a HIPAA violation? How do you build trust while boosting patient engagement? How do you implement strategies such as email personalization and secure email workflows without exposing sensitive patient data? Well, the answer lies in knowing well the privacy and security requirements of HIPAA, creating consent-based strategies, and adopting tools that were built with compliance in mind, including but not limited to encryption, access controls, and signed Business Associate Agreements (BAAs) features.
This guide will serve as your fully-fledged playbook for doing just that. Be it the marketing strategist at the healthcare provider, product lead building a patient-facing avenue, or compliance officer piloting communication through airtight channels, learn how to design personalized experiences compliant with regulations and impactful on outcomes. Transforming the nuances of de-identifying data and adopting HIPAA-compliant technologies for healthcare communications, we show how to value the benefits without compromising them.
What is HIPAA Compliance and why it Matter in Personalization
The Health Insurance Portability and Accountability Act (HIPAA) is a U.S. federal law enacted in 1996 to safeguard sensitive patient health information. At its core, HIPAA establishes rules for the collection, use, and protection of Protected Health Information (PHI), which includes any data that can be used to identify an individual in a healthcare context. This includes not just medical records, but also data like names, addresses, contact information, IP addresses tied to patient accounts, and even appointment reminders.
For organizations that handle PHI—such as hospitals, insurance providers, digital health platforms, and their vendors—HIPAA compliance is not optional. It involves a combination of administrative protocols, physical safeguards, and technical controls, including encryption, secure storage, access logging, and signed Business Associate Agreements (BAAs) with third-party service providers.
Why PHI Is in the Heart of the Privacy Discussion
PHI, or patients' protected health information, contains health data, which relates to a person's physical or mental condition; about providing healthcare; or regarding payment provision for healthcare services. PHI is different from personally identifiable information (PII), which has a more generic meaning and more use; PHI stands in the context of health and therefore is much more restricted.
This delineation is essential when having personalization strategies. For instance, other marketers in different industries may rely on browsing behavior, purchase history, or cookies, healthcare organizations should be extra careful. Something as seemingly innocent as customizing a subject line of an email with a treatment or diagnosis of a patient could constitute an unlawful disclosure of PHI if not authorized and secured correctly.
The Cost of Non-Compliance In a Personalization Context
Violations of HIPAA can cost an organization dearly-realistically, in financial, reputational, and legal terms. Offenses against HIPAA carry fines ranging anywhere from $100 to $50,000, with an annual cap of $1.5 million per type of violation. More importantly, mishandling patient data can destroy the trust and credibility of an organization when personalized communications reveal sensitive information.
Some of them include sending unencrypted email marketing messages that include PHI, using tracking technologies without approval, or partnering with platforms without signing a BAA. Even things that can be considered standard in digital marketing-such as A/B testing personalized web content-can lead to non-compliance if they include patient data and the right controls are not in place.
How HIPAA Shapes the Role of Marketers, Product Teams, and Designers
Besides affecting law and compliance officers, HIPAA also fundamentally requires the marketer, product team, and UX designer to work with completely different mindsets in a healthcare setting. For marketers, HIPAA limits how segmentation, retargeting, or email personalization could work. For product teams, it means that patient data security must be integrated at every level of the tech stack-from architecture to API-level controls. For designers, it requires user journeys that balance relevance and privacy, including opt-in consent flows, secure logins through personalization, and frictionless communications in healthcare that stay on the safe side legally.
In short, HIPAA-compliant personalization isn't just a legal checklist; it requires cross-disciplinary thinking where every personalization approach is assessed through a dual lens of user experience and regulatory integrity.
What Counts as Personalization in the HIPAA-Driven Environment
Personalization, in general, relates to making experiences relevant; however, in the healthcare space, it explicitly refers to keeping all such relevant experiences within the precincts of one of the most stringent privacy laws. This section discusses the types of personalization typically found in digital experiences, which techniques infringe on PHI(Public Health Information), and how to provide personalized experiences legally and ethically within HIPAA compliance.
Types of Personalization in Healthcare
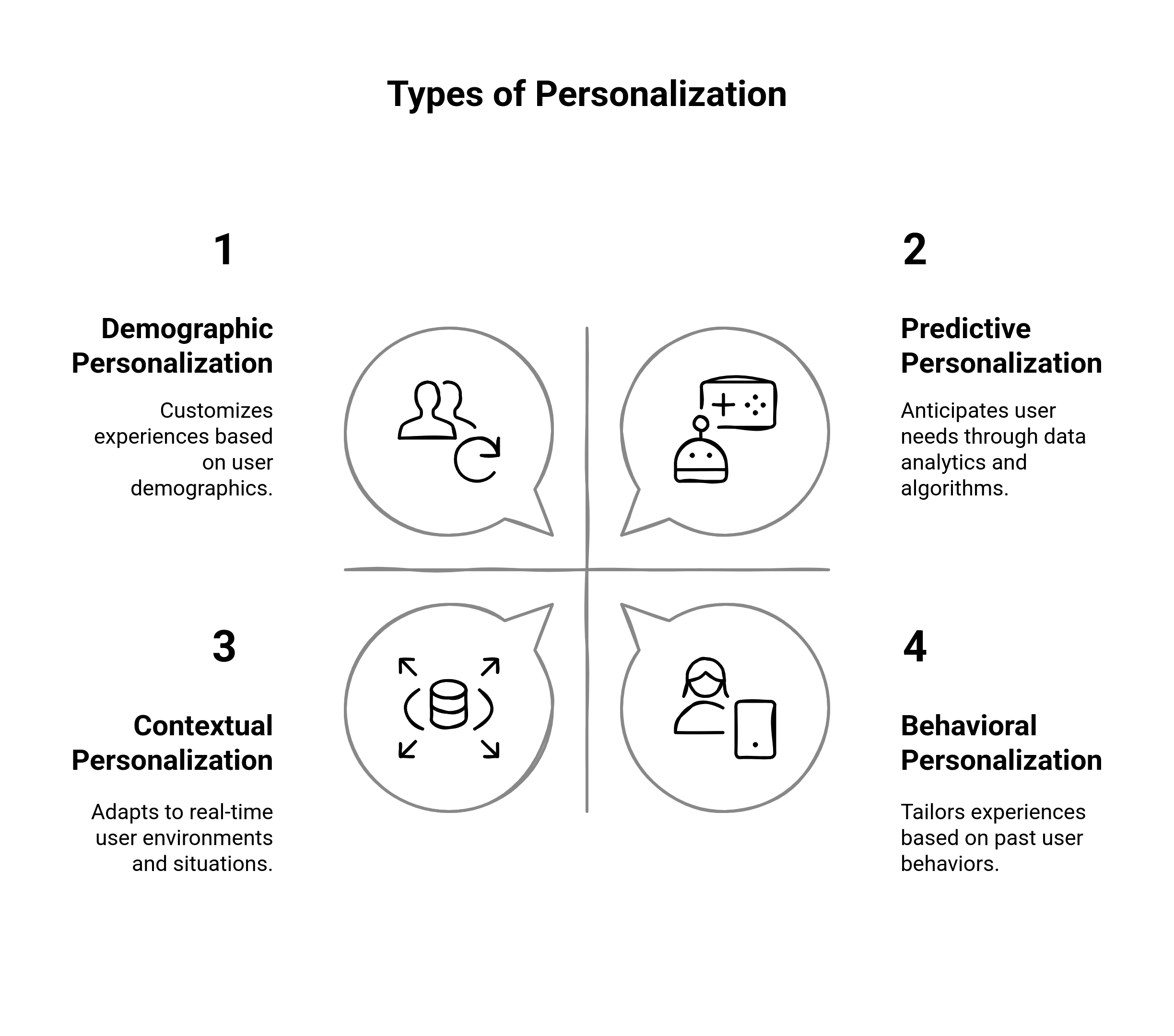
Within health care, personalization can be:
- Behavioral personalization: The tailoring of content based on actions taken in the past, such as login history, portal clicks, or appointment bookings.
- Contextual personalization: The customization of experiences based on device, time of day, or location, as with surfacing urgent care centers nearby.
- Demographic personalization: Using demographic data (e.g., whether a patient is male or female, or which insurance they are on) to customize content or suggestions.
- Predictive personalization: Algorithms predict what patients will need (e.g., a refill reminder sent because of the patient's medication history, or suggested wellness content based on managing their condition).
While all of these efforts can undoubtedly make patient engagement more meaningful, achieving a great experience or an egregious violation is entirely dependent on how data was collected, stored, and utilized.
Personalization That Does Involve PHI
Any personalization that incorporates or makes reference to individually identifiable health information is considered as PHI under HIPAA. Examples follow:
- Email marketing that includes a reference to medical conditions, diagnosis, or treatment.
- Appointment reminders that include details about the service type (e.g., "Your dermatology follow-up is scheduled for Friday.").
- Customizing portal dashboards based on clinical findings, lab results, or care plans.
- Push notifications for prescription refills or chronic condition management.
These are wonderful and highly effective means for improving healthcare communication, but because they involve protected health information, they must be implemented under very tight requirements: explicit patient consent, secure email systems, signed Business Associate Agreements (BAAs) with the vendors, and robust encryption for data at rest and in transit.
Personalization That Does Not Reference PHI
A few such tactics fall into the "safe" zone in association with regulations concerning PHI exclusion-
- Segregation of the website content based on broad behavioral patterns, such as "new versus returning visitor."
- Geographically based informational offer to a public audience that does not specify the user and does not tie them to a care history.
- Using such preference-based settings, the user specifically sets up (e.g., preferred language, preferred type of content).
- Providing general health education content based on non-sensitive definitions (for example, by age group or interests).
Caution is certainly warranted, however. It is possible to consider as PHI data that on its face does not appear sensitive (e.g., cookies, IP addresses, and device IDs) when linked to a user's interaction with a healthcare provider's digital properties.
What’s Permissible Under HIPAA With Proper Consent and Safeguards
The good news? Personalization is allowed under HIPAA, with the right protocols in place. If a patient gives valid, written authorization for the use of their data for communication, education, or outreach, the door to HIPAA-compliant personalization opens significantly wider. With a proper Business Associate Agreement, healthcare organizations can partner with platforms that enable secure email, audience segmentation, and even AI-driven personalization—so long as PHI is handled according to HIPAA’s Privacy and Security Rules.
To remain compliant, always ensure:
- Explicit opt-in consent for any marketing that includes PHI
- All platforms handling PHI have signed BAAs
- PHI is transmitted only over encrypted, secure channels
- A clear audit trail is maintained for personalized outreach
In short, the goal is not to avoid personalization, but to implement it intelligently. When done right, HIPAA-compliant personalization can boost patient engagement, reduce friction, and build lasting trust.
What PHI is and how it Affects Personalization Strategies
Understanding what constitutes PHI (Protected Health Information) is the cornerstone of any HIPAA-compliant personalization strategy. This section defines exactly what data is regulated under HIPAA, outlines common high-risk data sources, and clarifies the legal distinction between de-identified and anonymized information. You’ll also see examples of personalization that stay within the boundaries—and those that don’t.
What Counts as PHI Under HIPAA?
PHI refers to any health-related data that can be used—either directly or indirectly—to identify an individual. According to the U.S. Department of Health & Human Services (HHS), the following 18 identifiers qualify as PHI when tied to healthcare services, payments, or diagnoses:
- Name
- Address (all geographic subdivisions smaller than a state)
- Dates (birth, admission, discharge, death, etc.)
- Phone numbers
- Fax numbers
- Email addresses
- Social Security numbers
- Medical record numbers
- Health plan beneficiary numbers
- Account numbers
- Certificate/license numbers
- Vehicle identifiers and serial numbers
- Device identifiers and serial numbers
- Web URLs
- IP addresses
- Biometric identifiers (e.g., fingerprints, voice prints)
- Full-face photos and similar images
- Any other unique identifying number or code
When even one of these is linked to a health-related service or condition, it becomes PHI and falls under HIPAA regulation.
Common Types of Data Sources and Their Levels of Risk
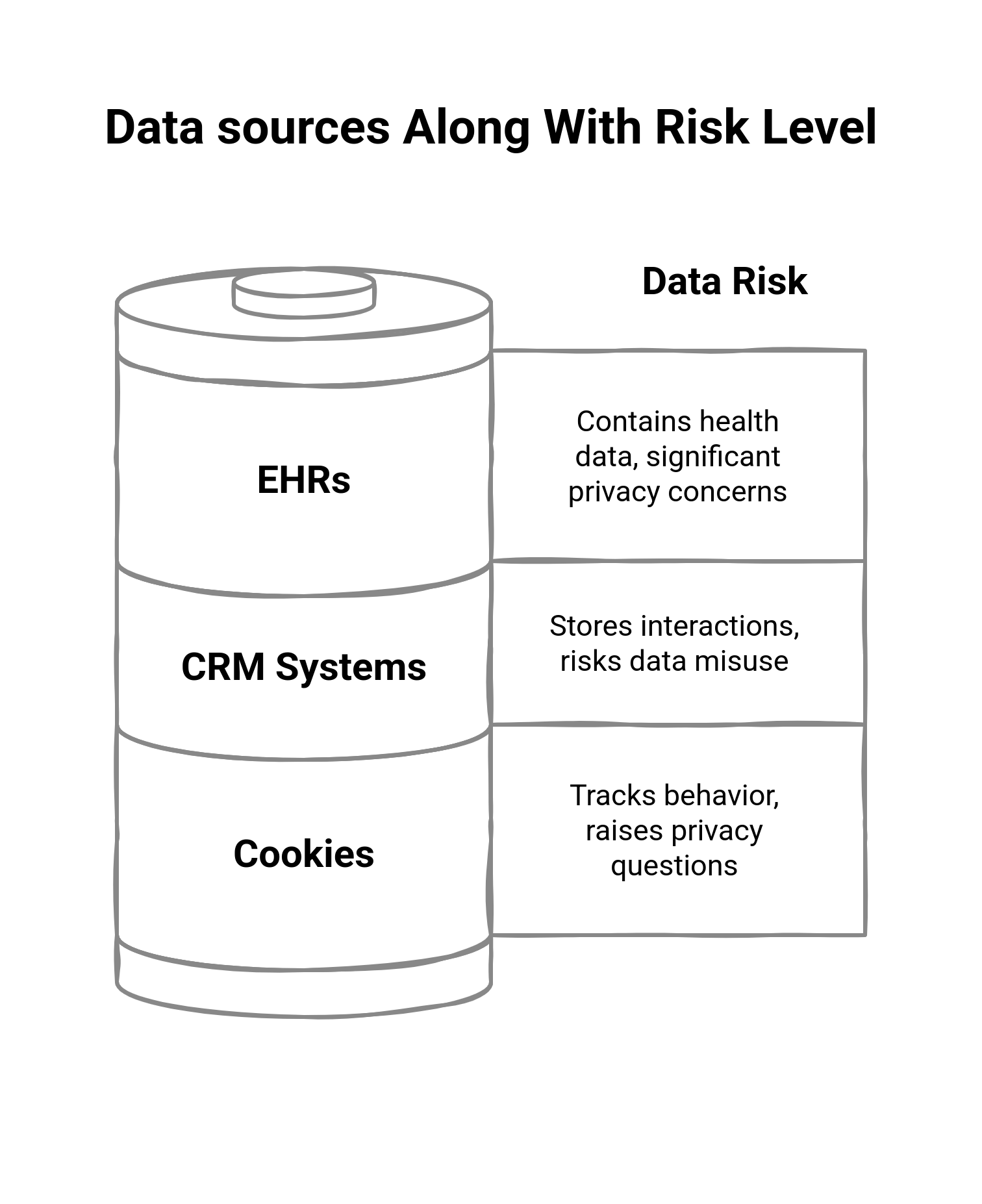
Most modern personalization draws upon multiple systems, many of which risk PHI exposure in case of mishandling.
- Electronic Health Records (EHRs): High risk, nearly always containing PHI.
- Customer Relationship Management (CRM) tools: High risk to medium risk depending on the data stored.
- Web behavior (e.g., login patterns, clickstreams): Risky if identified by patient identities.
- Cookies and tracking pixels: Have the potential to turn into PHI through their use on patient portals or other healthcare resources associated with identities.
An organization's greatest mistake would be to think that web analytics or behavioral data can be freely used within the organization. If a tool logs IP addresses on a site used for care management or health services, then those logs must be counted as PHI, especially with login data or email addresses under their records.
De-Identified Versus Anonymized Data: In Contrast
De-identification is the process by which HIPAA defines an individual as having removed all eighteen identifiers or certified by a qualified expert as posing a very low risk of re-identification. There are two approved procedures under HIPAA:
- Safe Harbor: Remove all 18 identifiers above.
- Expert Determination: A statistical analysis certifying that the data is no longer identifiable on an individual basis
Anonymization, while commonly used in marketing, is not a legal term under HIPAA. Data may be “anonymized” in marketing platforms, but still violate HIPAA if it contains linkable identifiers.
Safe vs. Unsafe Personalization Use Cases
Safe personalization (with safeguards or de-identification):
- Recommending general wellness content based on de-identified portal behavior
- Offering localized services based on ZIP code without linking to care history
- Customizing content based on user-selected preferences
Unsafe personalization (without consent or safeguards):
- Auto-populating emails with treatment or diagnosis information
- Using behavioral retargeting from a patient portal visit
- Syncing CRM data to ad platforms without a Business Associate Agreement (BAA)
Personalization in healthcare must be surgical: it’s not about what’s possible—it’s about what’s permissible.
How to Collect User Data for Personalization Without Violating HIPAA
HIPAA does not restrict collecting data but regulates its collection, storage, and usage. The section below details the avenues through which healthcare can collect the right kinds of data to power personalization while keeping the lines of compliance intact, from best practices for first-party data to HIPAA-approved consent language. The section will cover building compliant personalization pipelines.
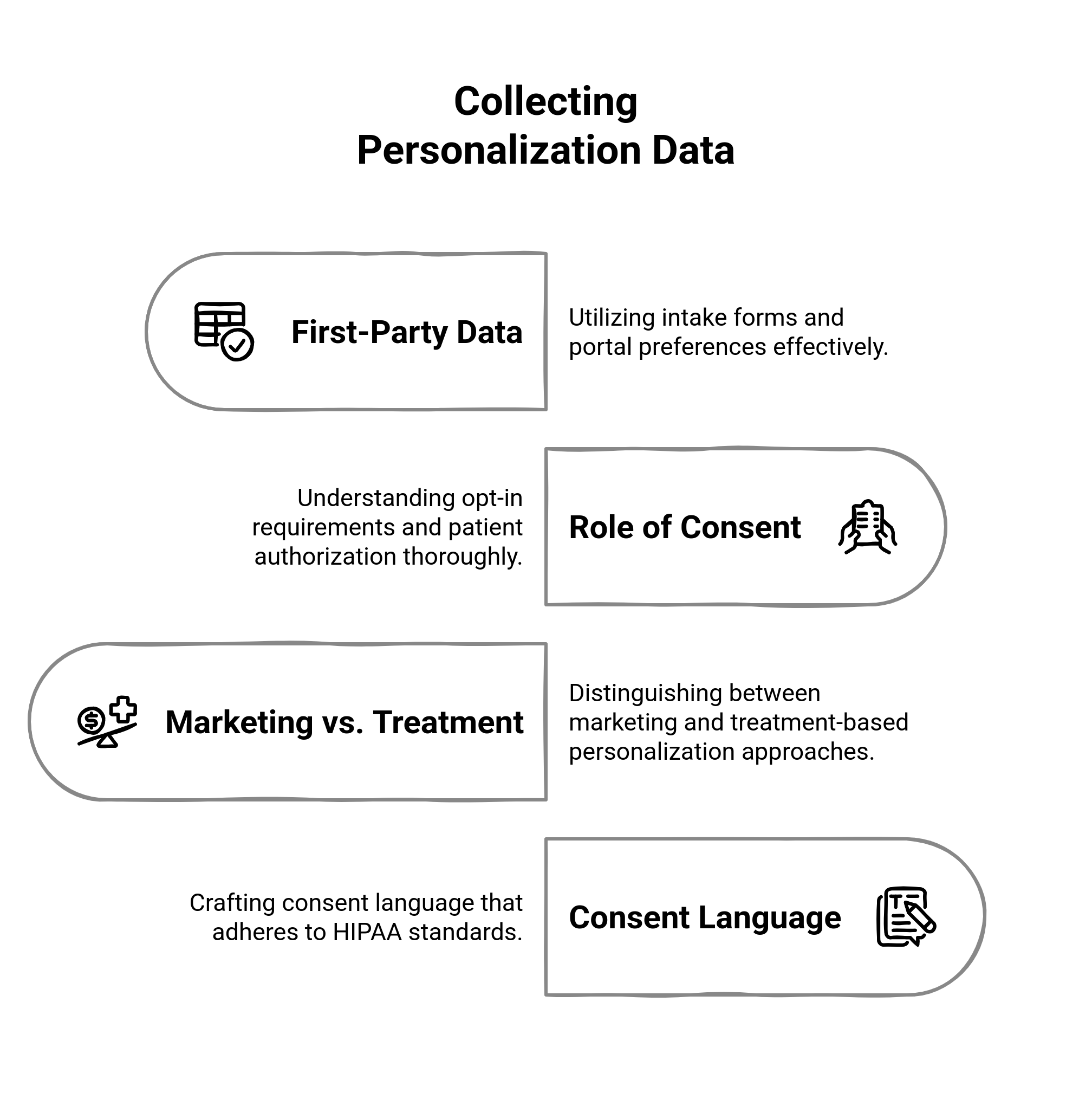
First-party Data
First-party data is by far the safest kind of data: what your users give you voluntarily and knowingly.
Patient-consented intakes for personalizing communication digitally
Preference centers on portals where they can choose topics of interest, preferred channels, and content types
Appointment survey feedback, having trajectories where subject to personalization.
Collecting first-party data is the only example of doing the personalization right because it is safe and patient-centred, hence lowering the risk of legal aspects and improving trust.
The Role of Consent During Opt-in
HIPAA requires explicit patient authorization written down for the use of PHI purposes attributable to marketing or communications beyond the treatment, payment, or operational functions (TPO). This fact is pertinent to:
Email blasts
Patient-retargeting
Automated workflows are set up to send messages according to clinical milestones
Consent must clearly articulate:
What data is being used
How will it be used
Who will it be shared with
How patients can opt out
Marketing vs Treatment-based Personalization
It helps to understand how HIPAA distinguishes between the two:
Treatment-based personalization: It is covered under the law, without needing any extra authorization. E.g., “Time to refill your blood pressure medication.”
Marketing-based personalization: Requires patient authorization. E.g., “Check out this new wellness product from our partners.”
If the message goes into promoting products and services without them being tied directly to the provider's treatment, and the provider is being paid to promote, then it becomes marketing, which falls under HIPAA and needs authorization.
Consent Language That Satisfies the HIPAA Standards
Here is an example of wording that is compliant with HIPAA regarding consent:
"By checking this box, I authorize [Provider Name] to send me health-related educational content and promotions using my personal health information. I understand this may include reminders, recommendations, or other personalized outreach based on my medical history. I may revoke this authorization at any time."
Your legal team should review all consent text, but it is critical that marketing, product, and compliance teams get aligned to ensure that consent mechanisms are present, clear, and properly logged.
HIPAA-Compliant Personalization Tools and Platforms
Personalization in the healthcare sector cannot rely on just any CRM, CDP, or marketing platform. To comply with HIPAA standards, all touchpoints-data collection, storage, activation, and communication-must be secured by an appropriate infrastructure, protocols, and vendor agreements. This section outlines compliant tools, what features to view, and how to decide between building custom or buying ready-made platforms.
Overview of HIPAA-Compliant CDPs, CRMs, and Marketing Platforms
Usually, healthcare organizations use the following systems on which they can build personalization within the frameworks of HIPAA:
- Customer Data Platforms (CDPs): A CDP collects and unifies first-party data from multiple sources (e.g., EHR, portals, forms) while ensuring PHI segmentation under HIPAA.
- Customer Relationship Management (CRM): Tracks patient interactions, preferences, and communications. Must allow access control and PHI encryption.
- Marketing Automation Platforms: They run email campaigns, allow behavioral triggers, and define patient journeys. That is all HIPAA-compliant email, personalization, secure email, and logging.
However, there are many common tools with no healthcare aspect. The absence of proper HIPAA protection-such as a BAA or encrypted workflows-means that a compliance violation could occur in a matter of seconds.
HIPAA Standards Compliance Platform: What Must You Look For?

In the evaluation of a CDP, CRM, or email tool, always consider platforms that have:
- A signed Business Associate Agreement (BAA): This is legally required if the platform stores, processes, or transmits PHI on your behalf.
- Audit trails and access logs: These must narrate who accessed patient data, when, and why—critical in an investigation or security audit.
- Role-based access control (RBAC): NO PHI should be accessed by unauthorized users. The platform should allow for granular user permissions.
- End-to-end encryption: Any data, whether being transmitted or at rest, must be encrypted using industry-standard AES-256, TLS 1.2+, for example.
- Management of consent and preferences: The tools must allow for capturing, storing, and honoring of patient consent, especially in email marketing.
In the absence of these amenities, no matter how advanced they may be, personalization tools are not qualified for HIPAA-compliant workflows.
Examples of Some HIPAA Compliant Personalization Tools
Here are some prominent platforms that allow HIPAA-compliant personalization solutions when the right configuration and agreements are in place:
- Salesforce Health Cloud: Specifically built for the healthcare profession with PHI management, patient journey mapping, and BAAs under Salesforce's offering.
- Twilio Segment (with HIPAA BAA): An advantageous CDP that would only support HIPAA-compliant data flows when set up properly and run under a signed BAA.
- Iterable (Enterprise HIPAA plan): Allows HIPAA-compliant email journeys and audience segmentation only with specific higher-level agreements.
- Custom-built solutions: Many enterprise healthcare providers build their own platforms to have higher control over patient data security and workflows.
How to Personalize Healthcare Experiences While Staying HIPAA Compliant
Personalizing healthcare experience does not stop at the login screen. Making the most of this potential with safeguards and strategies can provide benefits such as patient satisfaction, enhanced health outcomes, and reduced friction in care delivery. This section illustrates the personalization of patient experiences through web, e-mail, and mobile platforms without risk to patient data security.
Personalizing Web Content in Legitimate Ways
Web-based strategies for personalization can be applied in healthcare, but must be carefully fashioned around HIPAA. Some safety measures are:
Exhibiting location-based care suggestions using anonymous geo data, such as nearby clinics or appointment slots.
Patient education content could be recommended per de-identified browsing behavior or user preferences set through a secure portal.
Dynamic content (condition-specific FAQs, for example) could be displayed post-secure login to ensure PHI is not exposed on the public-facing page.
Do not trigger personalized content on generic pages unless the user is an authenticated one, and, for any retrieval of data linked to PHI, the communication should be encrypted.
Personalizing Emails and Notifications Safely
For email personalization to comply, one must put in the painstaking effort to replicate the three prerequisites: consent, content, and delivery infrastructure.
Secure email platforms such as Paubox or Virtru that encrypt messages containing PHI, including test results and care reminders.
Personalize messages based on treatment stage, such as sending post-visit follow-ups, medication refill reminders, or wellness tips according to a patient's condition.
Trigger notifications for flu shots, local health events, or availability of specialists based on location, but only if an individual has given their consent.
In advance of patient authorization, every personalized message using PHI must. Include a clear opt-out option and audit trails for compliance tracking.
Mobile application and Patient portal personalization
There's no denying that apps and patient portals are best when it comes to providing personalized experiences. They are usually accessed in an authenticated, secure environment.
Tailored user flows and dashboards depending on care milestones (e.g., recovery progress, future screenings, treatment plans).
Equipping Language preferences and access features for better engagement with diverse patients.
Give patients the opportunity to configure what types of content, form of communication, and type of appointments should be reflected in the portal.
Portals are designed to handle PHI by default; therefore, make sure that all portals comply with the HIPAA encryption standards and are created with role-based access control to restrict disclosure.
Examples of Compliant Personalization
- Cleveland Clinic sends secure post-visit summaries and relevant next steps via encrypted email after patient authorization.
- Mayo Clinic's patient app displays personalized care plans and health education modules based on diagnosis, only after login.
- One Medical uses location and preference data to surface nearby services, doctor availability, and flu shot reminders—all within a compliant, consent-driven framework.
These organizations show that HIPAA-compliant personalization is not only possible—it’s a differentiator in modern healthcare communications.
How to Secure Personalized Experiences Under HIPAA Rules
No personalization effort going through HIPAA is going to be whole without the proper technical ends. Whether it is customizing a dashboard or sending a mass emailing, security requirements must be embedded into the fundamental characteristics. This section narrates what every organization must do to make personalized experiences safe and legal.
Encryption: In Transit and At Rest
On-the-fasis conditions of HIPAA, PHI security strongly connects both the methods of keeping it in settings and during its transmission.
Use AES-256 encryption for data at rest, which includes databases, cloud storage, and backups.
Use TLS 1.2 or higher for data in transit, especially between APIs, web sessions, and email communications.
Secure email platforms automatically encrypt messages without requiring the recipient to set up extra passwords or portals, since these tools reduce friction and thereby boost patient engagement.
All the platforms used for personalization, a CDP or CRM, or a marketing automation tool, will have encryption built into their infrastructure.
Regular Audits and Training for Personalization Teams
Compliance is not a one-off checkbox task. Continuous education as well as auditing a campaign proactively are vital to ability sustain HIPAA-compliant personalization.
Plan internal HIPAA audits on personalization campaigns, email journeys, and platform usage on a quarterly to biannual basis.
Conduct HIPAA-specific training for marketing, product, and UX teams involved in designing and delivering personalized content.
Engage the compliance or legal team ahead of launching new campaigns or tech integrations.
Where compliance-first personalization is the culture, innovation never earns the right to breach patient trust or legal safety.
Role-Based Access Control and Authentication
For each team member to enjoy a truly personalized experience, he or she sometimes must be able to access patient information that warrants the implementation of RBAC.
Limit access to PHI to those members who require it (e.g., care coordinators, HIPAA-trained marketers).
Enforce MFA for all internal users accessing PHI-related systems.
Set up session timeouts and audit trails to prevent unauthorized access and data leakage from inactive sessions.
This principle of least privilege is not only designed to minimize internal risks but also to tightly control access to sensitive data.
Logging, Monitoring, and Incident Response
All systems handling any PHI personalization must have an audit log and monitoring.
Every time PHI is accessed, modified, or transmitted, it must be logged with timestamps and user IDs.
It will enable a real-time monitoring system to flag unusual patterns, such as bulk downloads or unauthorized logins.
Maintain a formal incident response plan that outlines procedures for breach investigation, reporting, and mitigation.
HIPAA wants evidence that organizations cannot simply comply with security practices but also ensure oversight.
Conclusion
As patient expectations evolve, healthcare organizations must rise to meet them, not just with innovation, but with integrity. HIPAA-compliant personalization isn’t about pulling back on digital experiences; it’s about designing them with discipline. From securing PHI and encrypting every message, to crafting consent-first email marketing campaigns and building compliant workflows into CRMs and CDPs, success lies in the details.
Done right, personalization becomes more than a tactic—it becomes a competitive advantage. It improves patient engagement, streamlines care delivery, and builds long-term trust in your brand. But it must always be underpinned by rigorous safeguards: access controls, audit trails, secure email infrastructure, and signed Business Associate Agreements (BAAs) with every vendor in your data ecosystem. At the heart of it all is a simple but powerful idea: patient data deserves the same care and attention as the patients themselves. When privacy and personalization go hand in hand, healthcare doesn’t just communicate—it connects.




